Trachea: The trachea is the tube that carries air from your throat to your lungs. It’s also called the windpipe.
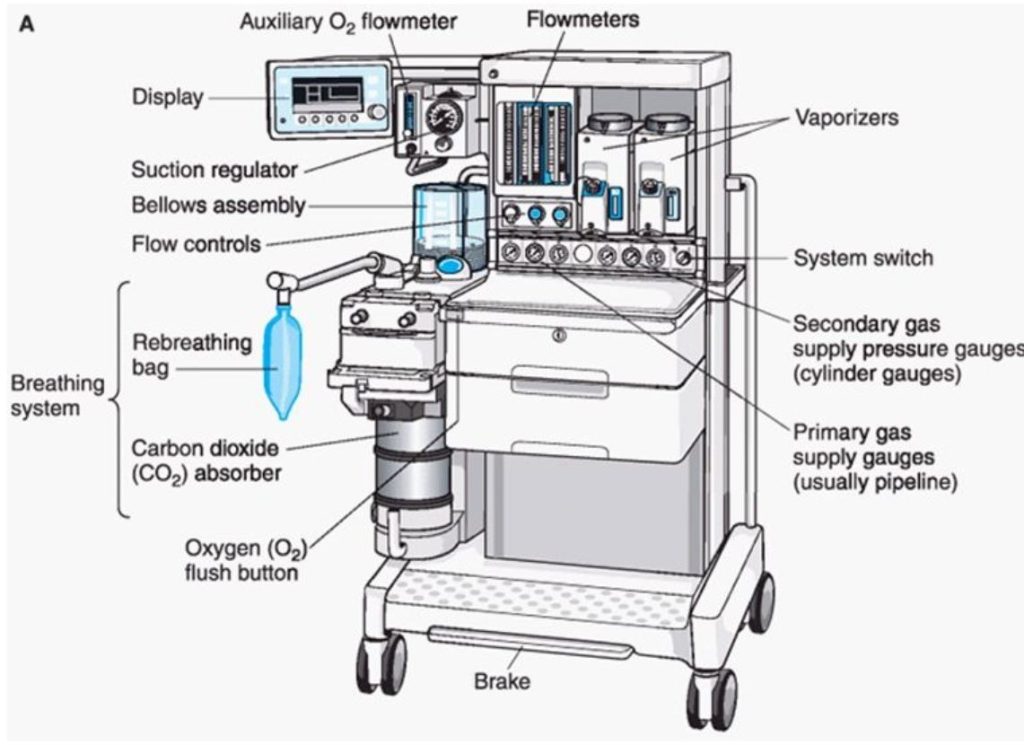
Anesthesia Machine: An anesthesia machine delivers gases, liquids, and medications to a patient during surgery. It also monitors the patient’s heart rate, blood pressure and breathing during surgery.
Anesthesia Machine Parts: There are four main parts to an anesthesia machine:
Gas
The trachea is the tube that connects the lungs to the rest of the body. The trachea is a part of the respiratory system. Tracheal intubation is inserting a tube into the trachea.
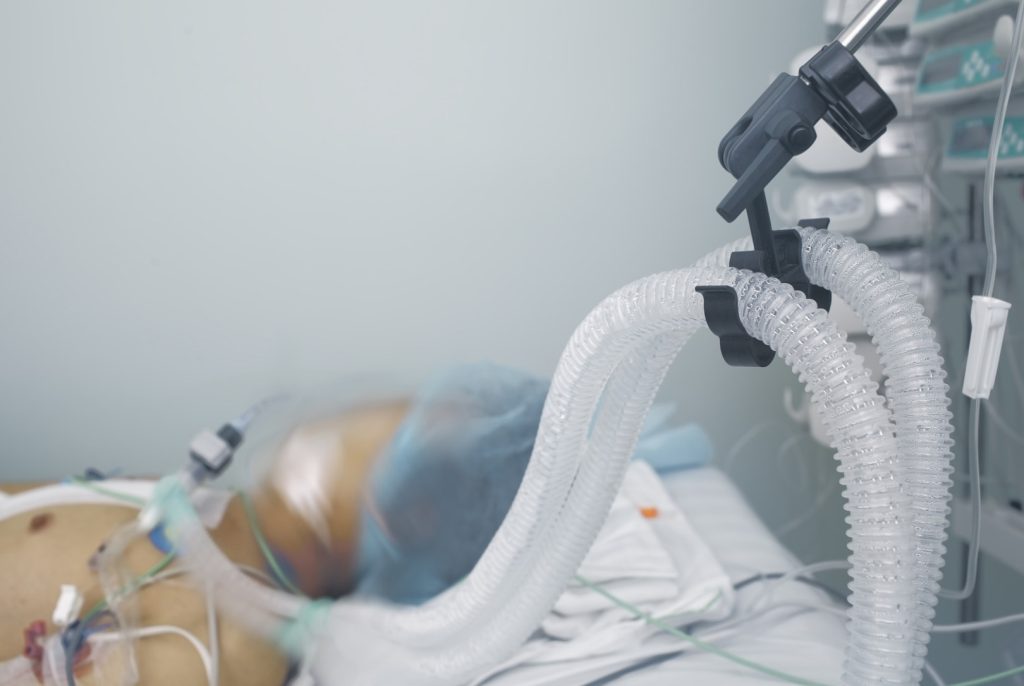
The endotracheal tube is a long, thin tube that is inserted into the trachea through the nose and down into the lungs. The endotracheal tube is connected to a filter, an in-line suction device, and a transport ventilation device.
When starting transport, leave the viral filter in place on the endotracheal tube and connect the filter to the transport ventilation device. Use in-line suction and nebulization devices. Clamp the endotracheal tube whenever it is disconnected from the filter to maintain a closed system.
Once a “high-quality” viral filter is in place on the endotracheal tube, they can disconnect the breathing circuit from the filter while moving a patient or to reconnect to a different ventilation device. The filter will reliably stop viruses exhaled by the patient from contaminating the room. Suctioning the endotracheal tube or administering nebulized medications is a unique problem.”
Valves
A valve is a mechanical device that controls the flow of fluid through a pipe by opening, closing, or partially obstructing it. There are many types of valves, including:
– Ball valves
– Butterfly valves
– Check valves
– Diaphragm valves
– Gate valves
– Globe valves
– Plug valves
The most common type of valve used in an anesthesia machine is a ball valve. A ball valve comprises a ball with a hole in the center that is connected to a handle. They placed the ball in front of an opening in the pipe. When the handle is turned, the ball rotates to either open or close the opening.
Source
The hospital pipeline is the primary gas source of an anesthetic machine. The pressure in the pipeline is about 50 pounds per square inch (psi). There is an oxygen flush that goes “straight shot” from the pipeline to the common gas outlet (which bypasses the vaporizers and flowmeters), at a rate of 35-75 liters per minute.
The OSHA website has links on Waste Anesthetic Gases (WAGs). According to the NIOSH recommendation, occupational exposure should be limited to 2 parts per million (ppm) halogenated agents (0.5 ppm if nitrous oxide is used), and not over 25 ppm nitrous oxide. You can read the 1977 NIOSH recommendation on waste gases here.
Tubing sizes: scavenger 19 or 30 mm, ETT or common gas outlet (CGO) 15 mm, breathing circuit 22 mm.
Space
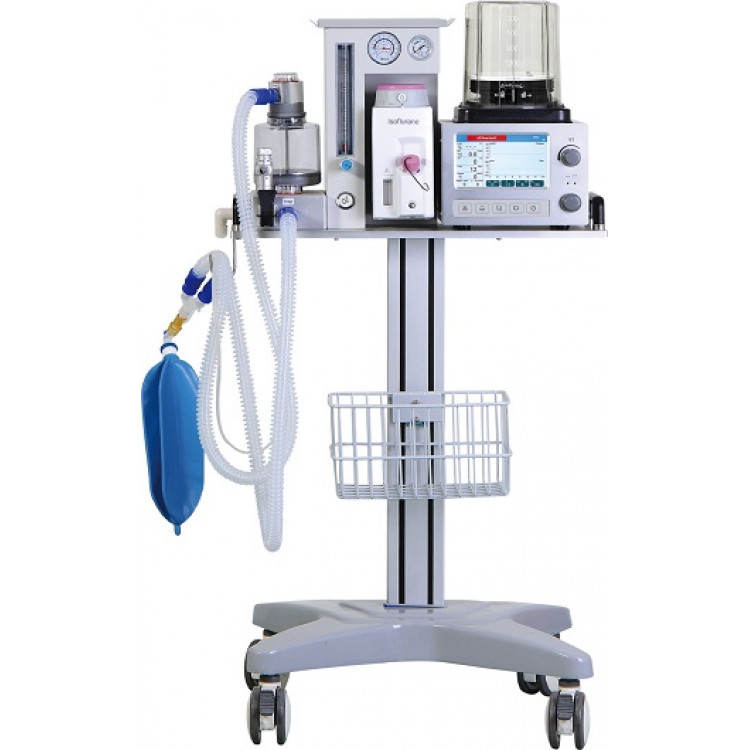
The crustation™ 650c Anesthesia Machine is a compact system designed for pendent or wall mount — an ideal solution for induction rooms where floor space is limited. The machine has a filter placed between the breathing circuit and the patient’s airway that adds to respiratory dead space. If we cannot place a filter between the breathing circuit and the patient’s airway, then place a viral filter at the end of the expiratory limb at the connection to the anesthesia machine.
Features
Anesthesia machines improve patient safety. The new wave of anesthesia machines are more reliable and capable than basic pneumatic-mechanical designs. Most of the machines are based on pressure-controlled breaths, and allow for the addition of PEEP. Some machines include pressure control ventilation (PCV), pressure control ventilation with volume guarantee (PC-VG or outflow), synchronized intermittent mandatory ventilation (SIMV) with pressure- or volume-controlled breaths, pressure support ventilation (PSV), continuous positive airway pressure (CPAP), bi-level positive airway pressure (BiPAP), and airway pressure release ventilation (APRV).
View
The ICU Advantage is a website that provides information about anesthesia machines. The website breaks down how an anesthesia machine works by component. It explains the function of each part and how it works with other parts to provide anesthesia. The website also provides information about delivery systems and workstations for anesthesia machines.
Transmission
Terms
Anesthesia machine – a machine used to provide anesthesia during medical procedures. The anesthesia machine has three main parts: the breathing system, the delivery system, and the workstation.
Anesthetic gas – a gas used in an anesthesia machine. There are many different types of anesthetic gases, but the most common ones are carbon dioxide, nitrous oxide, and soda lime.
Carbon dioxide – a gas that is often used in an anesthesia machine. Carbon dioxide is a colorless, odorless gas that is produced by the body during respiration. It is also used as a coolant in some Anesthesia machines.
Breathing system – the system used to deliver the anesthetic gas to the patient. The breathing system comprises an airway, a mask, and tubing. The airway is a tube that goes from the patient’s mouth to the lungs. The mask is placed over the patient’s nose and mouth and delivers the anesthetic gas to them. The tubing connects the mask to the Anesthesia machine.
Delivery system – the system used to deliver the anesthetic gas to the patient’s body. The delivery system consists of a valve, a regulator, and a flowmeter. The valve controls the flow of gas to the patient. The regulator controls the pressure of the gas. The flowmeter measures the amount of gas that is being delivered to the patient.
Nitrous oxide – a gas used in anesthesia machines and as an analgesic. Nitrous oxide is a colorless, odorless gas that is produced by the body during respiration. It is also used as a coolant in some Anesthesia machines.
Soda lime – a type of anesthetic that is often used in surgery. Soda lime is a mixture of calcium hydroxide and sodium hydroxide. It absorbs carbon dioxide and water vapor from the air, making it an ideal anesthetic for surgeries that involve high levels of carbon dioxide production.
Gases
Anesthesia machines use gases to power different parts of the machine. The most common gases used are oxygen and nitrous oxide. The machine is designed to maintain the correct proportion between flows of these two gases.
The machine is also designed to be conceptualized in a Supply, Processing, Delivery & Disposal model. This means that the machine takes in gas from a tank, processes it, and then delivers it to the patient. Once the patient has exhaled the gas, it is then disposed of properly.
Circuits
Anesthesia machines have circuits that keep drugs and equipments like laryngoscopes and endotracheal tubes. The circuits are concealed by a metal top for keeping drugs and equipments safe. A table top has been created so that there is a space for monitors and other equipment.
Vaporizer
A vaporizer is a device that heats a liquid to produce a gas, which the user then inhales. Vaporizers are used to deliver inhalant anesthesia. The Tec TM 6 Plus vaporizer is a sophisticated and easily controllable electronic vaporizer that allows you to deliver Desflurane with confidence. The VetFlo vaporizers are traditional veterinary anesthesia systems that allow for the proper, safe, and effective delivery of inhalant anesthesia for rodents.
Work
Anesthesia machines are designed to provide a safe, efficient, and comfortable delivery of anesthesia gases to patients. The basic pneumatic-mechanical design of the anesthesia gas machine had become familiar to a generation of providers. These delivery systems are designed from the start to integrate all monitoring, advanced ventilation, electronic anesthesia record, and microprocessor controls. Most are based on pressure controlled breaths, and allow the addition of PEEP (not all modes are available on every model). They also improve accuracy in delivered tidal volumes in volume-control mode (VCV), but this mode is used much less frequently at present.
Meter
A flow meter is a device used to measure the flow of gas. Flow meters are made of borosilicate glass Pyrex. Flow meters have a single taper or a double taper. When there are separate flow meter tubes for low flows and high flows for the same gas then the tubes are single tapered. If there is a single tube for the gas then it is double tapered.
Format
Tube
The endotracheal tube is a tube that is inserted into the patient’s airway to allow them to breathe.
The endotracheal tube must be connected to a filter in order to prevent viruses from escaping and contaminating the room. Once a “high-quality” viral filter is in place on the endotracheal tube, the breathing circuit can be disconnected from the filter while moving a patient or to reconnect to a different ventilation device. The filter will reliably stop viruses exhaled by the patient from contaminating the room. Suctioning the endotracheal tube or administering nebulized medications is a unique problem. If suctioning is expected, a closed suction system (like those used in intensive care) should be placed between the endotracheal tube and filter as soon as the endotracheal tube is inserted. In line nebulizers will need to be placed on the patient side of the filter to deliver medication effectively.”



![The [Complete] Guide to Buying Anesthesia Machines](https://www.anesthesia-news.com/wp-content/uploads/2022/08/anesthesiamachine3.jpg)

![How to Find the [PEEP Valve] on an Anesthesia Machine](https://www.anesthesia-news.com/wp-content/uploads/2022/09/peep-valve.jpg)